Meet the families who have been impacted by Love Adelyn.
Our hearts are blessed to be a small part of their journey.
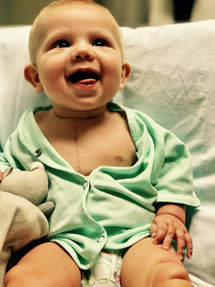
Elliot's Story written by his mother Rachel
Elliot was diagnosed with HLHS after a routine ultrasound revealed something was wrong with his heart We were sent to UNMC where we had more intensive ultrasound and then Children's to meet the team there and make a plan.Elliot was born 08/09/12 at UNMC at 38 weeks and taken right away to Children's where he then stayed in the NICU until his 1st open-heart surgery (Norwood) at 5 days old. He stayed in the hospital another 2 weeks as he learned to eat without the NG tube. He had his next cath at 6 months which revealed it was time for his 2nd surgery ( Glen) which was done in Feb of 2013. He stayed in the hospital 3 weeks recovering from some vocal cord damage and oral aversion.
Then right before his 1st birthday in July of 2013 we noticed that he was acting more tired, was a bit more puffy and a lot more "blue" in his extremities. He had a check-up with our family MD in Grand Island and she did a chest x-ray which revealed that his heart was enlarged. Children's was consulted and we made a trip to Omaha the next day where they diagnosed Elliot with the beginning stages of heart failure. He was then admitted and started on medication to help things.
We were introduced to the Heart Failure Cardiologist at the time, Dr. Steven Kindel. Elliot stayed in the hospital about a week taking the new medication and seemed to respond well so we was sent home. Fast forward a few months and we started to notice a decline again. We went back to our family practitioner who did another x-ray on his heart and showed concerns. It just to happened that Dr. Danford from Children's was here in Grand Island doing his out-patient clinic so he was called to consult. We then headed over to him where he did a echo. He then said that we needed to get to Children's asap as Elliot was declining and would need to start the process for transplant.
He was admitted October 15, 2013....never forget that day. He was placed on Milrinone IV to help reduce the stress of his heart and place on the transplant list as a 1A, the highest priority as he was required to stay inpatient. Mark and I took turns staying with Elliot and our daughter at home (2 1/2 hours away) who had just started Kindergarten that fall. The weekend were the best times as we reunited together in the hospital, making the most of our situation. We celebrated Halloween, Thanksgiving, Christmas, and New Years...waiting for his new heart.
Fiftteen minutes later our phone rang and it was the transplant coordinator telling us that Elliot had a offer for a heart...this was risky as he had just suffered a stroke...but it was a good match so we took it! Everything went well with transplant and just after Dr. Hammel sewed in his new heart, it started beating. 01/14/14- our son was saved by his angel heart, which just so happens to be Dr. Hammel birthday as well....
Elliot has done very well with his new heart. He did develop 3rd stage liver disease but that is kind of a mystery for his team. He had a renal-spleenal shunt surgery April 2016 to help reroute some of the blood flow around the liver which has greatly helped. He also had a stent placed in his IVC this March as he had a narrowing which couldn't be corrected with balloon angioplasty.
Then right before his 1st birthday in July of 2013 we noticed that he was acting more tired, was a bit more puffy and a lot more "blue" in his extremities. He had a check-up with our family MD in Grand Island and she did a chest x-ray which revealed that his heart was enlarged. Children's was consulted and we made a trip to Omaha the next day where they diagnosed Elliot with the beginning stages of heart failure. He was then admitted and started on medication to help things.
We were introduced to the Heart Failure Cardiologist at the time, Dr. Steven Kindel. Elliot stayed in the hospital about a week taking the new medication and seemed to respond well so we was sent home. Fast forward a few months and we started to notice a decline again. We went back to our family practitioner who did another x-ray on his heart and showed concerns. It just to happened that Dr. Danford from Children's was here in Grand Island doing his out-patient clinic so he was called to consult. We then headed over to him where he did a echo. He then said that we needed to get to Children's asap as Elliot was declining and would need to start the process for transplant.
He was admitted October 15, 2013....never forget that day. He was placed on Milrinone IV to help reduce the stress of his heart and place on the transplant list as a 1A, the highest priority as he was required to stay inpatient. Mark and I took turns staying with Elliot and our daughter at home (2 1/2 hours away) who had just started Kindergarten that fall. The weekend were the best times as we reunited together in the hospital, making the most of our situation. We celebrated Halloween, Thanksgiving, Christmas, and New Years...waiting for his new heart.
Fiftteen minutes later our phone rang and it was the transplant coordinator telling us that Elliot had a offer for a heart...this was risky as he had just suffered a stroke...but it was a good match so we took it! Everything went well with transplant and just after Dr. Hammel sewed in his new heart, it started beating. 01/14/14- our son was saved by his angel heart, which just so happens to be Dr. Hammel birthday as well....
Elliot has done very well with his new heart. He did develop 3rd stage liver disease but that is kind of a mystery for his team. He had a renal-spleenal shunt surgery April 2016 to help reroute some of the blood flow around the liver which has greatly helped. He also had a stent placed in his IVC this March as he had a narrowing which couldn't be corrected with balloon angioplasty.
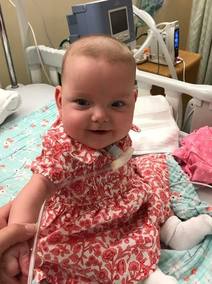
Abel's Story written by his mother Wendy
Abel was born on January 24th, 2017 at Children’s Hospital. He looked normal, amazing in fact. You would never guess in a million years that he had a critical heart condition. His first open heart surgery was at six days old. It was a planned surgery and the doctors were happy with the outcome. A few days later Abel’s tricuspid valve began to leak and he was faced with another surgery before two weeks old. The repair went well. The doctors even surprised themselves with the outcome. We were overjoyed! On February 23rd we went home. We were scared yet hopeful and ready to find our new normal. He was on several different medications three times daily. Besides the typical fussiness and inconsistent sleep patterns, it seemed like Abel was doing great. We had our first cardiology outpatient appointment on March 22nd and were checked in immediately after the doctors saw the results of Abel’s echocardiogram. His heart was failing.
Everything seemed to move really fast and then really slow at this point….and looking back now, I can’t believe where we are today.
After Abel was diagnosed with heart failure the team simply mentioned the word transplant but we found ourselves head first in the process meeting with the transplant team almost daily and filling out mountains of paperwork. Abel was considered “critically stable.” How is that a thing?! They almost even sent us home! These weeks seemed like years. Thankfully we had Children’s Hospital in our backyard and family close enough to visit daily. Abel was never alone. It was the most important thing we could do for him. We were in the hospital waiting for 25 days before any decision was made about Abel’s future. On April 10th the cardiac team decided that they would list him on April 20th PENDING INSURANCE APPROVAL. I can’t tell you how many times I heard those words. It was infuriating. Why wait? We were confused but little did we know it was the biggest blessing we could have hoped for. Abel suffered a massive stroke sometime around then and began having seizures on April 13th. If Abel had been on the list at this time they would have pulled him off because of his health deterioration. Even though we wanted him listed more now then ever we had to be patient. We had to continue to tell ourselves and each other everything was going to be fine. We were tested with this in the highest degree when Abel coded On April 18th and was put on ECMO. How much more could this little boy take?
The cardiac team was now faced with another challenge in Abel’s case. Some of the surgeons wanted to list him immediately, others wanted to wait. This particular chain of events had never happened at Children’s in Omaha or anywhere else for that matter. There was no research done on children who had experienced a massive stroke and what time frame was safe for them to have a transplant. In adults it was three weeks but children are completely different. On April 21st the team decided to take a risk and list Abel. He was still on ECMO and in a very bad place. Transplants are not typically done while the patient is on ECMO but they decided to roll the dice.
After several attempts to wean Abel off life support he was finally successful. He spent 8 days there regaining his strength and preparing for the greatest day of his life. On May 18th we got word that Abel had a match…he was getting a new heart.
This was the best day of our lives yet the worst day for some other family. We never lost sight of the fact that someone had to lose their life in order for Abel to live his. We’ve thought about this endlessly. Hoping that the donor family will want to meet Abel someday and see how their son or daughter blessed us with the greatest gift we can never repay. We can only promise them that his heart will not be wasted. We will take care of it completely and love it endlessly. It will have the most full life possible on this second chance.
We have been home for a few months now and Abel is thriving. He’s improving everyday and “catching up” faster than you would ever believe. He continues to impress every doctor, surgeon, therapist, and grandma and grandpa every time he sees them. He is truly a miracle.
Everything seemed to move really fast and then really slow at this point….and looking back now, I can’t believe where we are today.
After Abel was diagnosed with heart failure the team simply mentioned the word transplant but we found ourselves head first in the process meeting with the transplant team almost daily and filling out mountains of paperwork. Abel was considered “critically stable.” How is that a thing?! They almost even sent us home! These weeks seemed like years. Thankfully we had Children’s Hospital in our backyard and family close enough to visit daily. Abel was never alone. It was the most important thing we could do for him. We were in the hospital waiting for 25 days before any decision was made about Abel’s future. On April 10th the cardiac team decided that they would list him on April 20th PENDING INSURANCE APPROVAL. I can’t tell you how many times I heard those words. It was infuriating. Why wait? We were confused but little did we know it was the biggest blessing we could have hoped for. Abel suffered a massive stroke sometime around then and began having seizures on April 13th. If Abel had been on the list at this time they would have pulled him off because of his health deterioration. Even though we wanted him listed more now then ever we had to be patient. We had to continue to tell ourselves and each other everything was going to be fine. We were tested with this in the highest degree when Abel coded On April 18th and was put on ECMO. How much more could this little boy take?
The cardiac team was now faced with another challenge in Abel’s case. Some of the surgeons wanted to list him immediately, others wanted to wait. This particular chain of events had never happened at Children’s in Omaha or anywhere else for that matter. There was no research done on children who had experienced a massive stroke and what time frame was safe for them to have a transplant. In adults it was three weeks but children are completely different. On April 21st the team decided to take a risk and list Abel. He was still on ECMO and in a very bad place. Transplants are not typically done while the patient is on ECMO but they decided to roll the dice.
After several attempts to wean Abel off life support he was finally successful. He spent 8 days there regaining his strength and preparing for the greatest day of his life. On May 18th we got word that Abel had a match…he was getting a new heart.
This was the best day of our lives yet the worst day for some other family. We never lost sight of the fact that someone had to lose their life in order for Abel to live his. We’ve thought about this endlessly. Hoping that the donor family will want to meet Abel someday and see how their son or daughter blessed us with the greatest gift we can never repay. We can only promise them that his heart will not be wasted. We will take care of it completely and love it endlessly. It will have the most full life possible on this second chance.
We have been home for a few months now and Abel is thriving. He’s improving everyday and “catching up” faster than you would ever believe. He continues to impress every doctor, surgeon, therapist, and grandma and grandpa every time he sees them. He is truly a miracle.
Marlys' Story written by her mother Rachel
December 29, 2016 was a nice, sunny winter day. My parents were in town for the day and I went to work, thinking I would leave a little early to spend some time with them. Around 8:45, after discovering some blood, I drove myself to St. Elizabeth's, where I was admitted to L&D. After many hours of waiting and a few long ultrasounds, they took me back for an emergency C-Section.
I was 25 weeks along. Marlys Marie arrived at 4:52 pm. She weighed 1 pound, 12 ounces and was 12 1/2 inches long. She was tiny and perfect, even with a hundred wires attached to her and a tube & vent helping her breathe. When she was three days old, a nurse discovered a skin irritation on her right side, thinking it was caused by one of the sensors attached to her. It continued to get worse, it was biopsied and experts around the country were consulted.
The morning of January 11 our doctors at St. E's said Marlys would be transferred to Children's in Omaha. By 3 pm, we were in the smallest NICU room watching as numerous teams came to look at Marlys and her wound. Surgery was scheduled for 9 pm that evening. My childhood minister & family friend baptized Marlys by phone late that evening, with Justin, sprinkling water on her isolette. The admitting doctor gave Marlys a less then 20% chance of surviving. Her surgery was the scariest hours of my life. That surgery included removing two infected ribs and left her chest wall open.
Two days later, the surgeons went back in to do another debridement and remove another partial rib. Zygomycosis was the name of her fungal infection and is usually found in cancer patients due to their compromised immune systems. There was no research on how to treat someone as young & tiny as Marlys. A course of two anti fungal meds were given for the next five months. She got daily visits from both the surgical & infectious disease teams. She will most likely require additional surgeries as she grows to reconstruct her chest wall.
The next few weeks were long, as all we could do was wait for Marlys to grow & heal. March 19, Marlys was extubated for the first time and we got to hear her tiny voice. Due to her long intubation & poor lung development, Marlys developed BPD & pulmonary hypertension. After four weeks of no movement on vent settings, one more intubation and an extubation, the decision was made for Marlys to get a Trach and g-tube on April 21. Justin & I jumped right in, learning the trach life. The home vent was tried, with no success. One of the doctors described it as going from a BMW to a Ford. Finally, the first week of June, Marlys got on the home vent and liked it. We also go to try bottle feeding & breastfeeding for the first time. A care conference was held to discuss the next steps.
The next step was a move back to Lincoln to Madonna Rehabilitation Hospital on June 27. Marlys was 180 days old. Leaving the NICU was bittersweet, we wanted to leave, but we were leaving an amazing, loving, caring team of nurses, doctors & therapists. I decided to go home & sleep in my own bed the night of June 29. At 2:17 am, Madonna called us, Marlys' trach had somehow come out and it took 10 minutes of CPR to get her back. We met Marlys at Bryan East, where she was awake. After consulting her doctors at Children's, Marlys went back to Madonna.
Over the next few months, Marlys worked so hard during all 3 plus hours of therapy a day. Justin & I were anxious to take our little girl home, but we needed night nursing. Somehow, the stars aligned & prayers were answered in late September; home nursing had been found! On November 1, 2017, at 307 days old, Marlys got to go home!
I was 25 weeks along. Marlys Marie arrived at 4:52 pm. She weighed 1 pound, 12 ounces and was 12 1/2 inches long. She was tiny and perfect, even with a hundred wires attached to her and a tube & vent helping her breathe. When she was three days old, a nurse discovered a skin irritation on her right side, thinking it was caused by one of the sensors attached to her. It continued to get worse, it was biopsied and experts around the country were consulted.
The morning of January 11 our doctors at St. E's said Marlys would be transferred to Children's in Omaha. By 3 pm, we were in the smallest NICU room watching as numerous teams came to look at Marlys and her wound. Surgery was scheduled for 9 pm that evening. My childhood minister & family friend baptized Marlys by phone late that evening, with Justin, sprinkling water on her isolette. The admitting doctor gave Marlys a less then 20% chance of surviving. Her surgery was the scariest hours of my life. That surgery included removing two infected ribs and left her chest wall open.
Two days later, the surgeons went back in to do another debridement and remove another partial rib. Zygomycosis was the name of her fungal infection and is usually found in cancer patients due to their compromised immune systems. There was no research on how to treat someone as young & tiny as Marlys. A course of two anti fungal meds were given for the next five months. She got daily visits from both the surgical & infectious disease teams. She will most likely require additional surgeries as she grows to reconstruct her chest wall.
The next few weeks were long, as all we could do was wait for Marlys to grow & heal. March 19, Marlys was extubated for the first time and we got to hear her tiny voice. Due to her long intubation & poor lung development, Marlys developed BPD & pulmonary hypertension. After four weeks of no movement on vent settings, one more intubation and an extubation, the decision was made for Marlys to get a Trach and g-tube on April 21. Justin & I jumped right in, learning the trach life. The home vent was tried, with no success. One of the doctors described it as going from a BMW to a Ford. Finally, the first week of June, Marlys got on the home vent and liked it. We also go to try bottle feeding & breastfeeding for the first time. A care conference was held to discuss the next steps.
The next step was a move back to Lincoln to Madonna Rehabilitation Hospital on June 27. Marlys was 180 days old. Leaving the NICU was bittersweet, we wanted to leave, but we were leaving an amazing, loving, caring team of nurses, doctors & therapists. I decided to go home & sleep in my own bed the night of June 29. At 2:17 am, Madonna called us, Marlys' trach had somehow come out and it took 10 minutes of CPR to get her back. We met Marlys at Bryan East, where she was awake. After consulting her doctors at Children's, Marlys went back to Madonna.
Over the next few months, Marlys worked so hard during all 3 plus hours of therapy a day. Justin & I were anxious to take our little girl home, but we needed night nursing. Somehow, the stars aligned & prayers were answered in late September; home nursing had been found! On November 1, 2017, at 307 days old, Marlys got to go home!